Post Inflammatory Erythema: Causes & Treatment
Understanding Post Inflammatory Erythema: Your Guide to Treating Red Acne Marks
If you’ve ever battled a stubborn pimple, you’re likely familiar with the frustrating mark it can leave behind long after the inflammation has subsided. However, not all of these residual marks are the same.
While many people are aware of post-inflammatory hyperpigmentation (dark spots), a condition called post inflammatory erythema (PIE) is a common, yet often misunderstood, cause of persistent red or pink marks. This guide will explain what PIE is, how to treat it, and how to prevent it from occurring.
What is Post Inflammatory Erythema (PIE)?
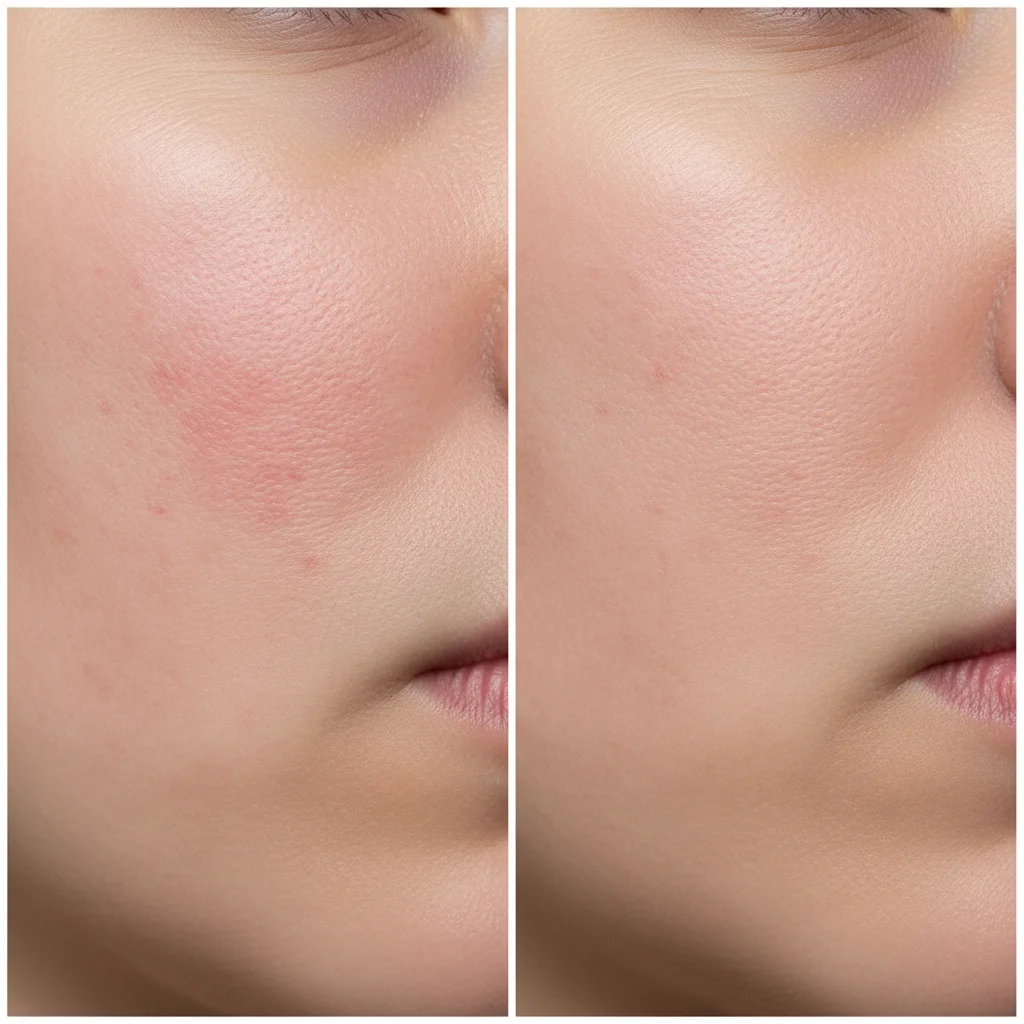
Post inflammatory erythema refers to the flat, red, pink, or purplish marks that remain on the skin after an inflammatory acne lesion has healed. Unlike hyperpigmentation, which involves an excess of melanin (pigment), PIE is a vascular issue.
Essentially, the inflammation from the acne causes damage to the tiny capillaries and blood vessels near the skin’s surface. This damage leads to dilated capillaries and an increased blood flow to the area, resulting in the visible red discoloration.
Consequently, PIE is most common in individuals with lighter skin tones and is frequently associated with inflammatory acne types like papules, pustules, and cysts. It’s crucial to distinguish PIE from hyperpigmentation because the treatment approaches are fundamentally different.
PIE vs. Post-Inflammatory Hyperpigmentation (PIH): Key Differences
Because they can appear similar to the untrained eye, understanding the distinction is the first step toward effective treatment. The table below outlines the primary differences.
| Feature | Post Inflammatory Erythema (PIE) | Post-Inflammatory Hyperpigmentation (PIH) |
|---|---|---|
| Primary Cause | Vascular damage and dilated capillaries. | Excess melanin production triggered by inflammation. |
| Color | Red, pink, or purple. | Brown, tan, black, or grayish. |
| Skin Tone Prevalence | More common in fair to light skin tones. | More common in medium to dark skin tones (Fitzpatrick III-VI). |
| Response to Pressure | The redness may blanch (turn white) briefly when pressed. | Color remains unchanged when pressed. |
| Common Treatments | Vascular lasers, intense pulsed light (IPL), topical niacinamide, azelaic acid. | Topical retinoids, vitamin C, hydroquinone, chemical peels, laser toning. |
What Causes Post Inflammatory Erythema?
The root cause of PIE is inflammation. When a pimple forms, the body’s immune response sends blood and inflammatory cells to the site to fight infection and repair tissue. This process can unfortunately damage the delicate capillary walls. Several factors can increase your risk of developing PIE:
- Severe Inflammatory Acne: The more severe the initial lesion, the greater the inflammation and potential for vascular damage.
- Picking or Squeezing Pimples: This traumatic manipulation significantly worsens inflammation and is a major contributor to PIE. It’s one of the worst habits for your skin’s recovery.
- Sensitive or Thin Skin: Skin that is naturally more delicate may have capillaries that are more prone to damage.
- Underlying Skin Conditions: Conditions like rosacea, which already involve vascular sensitivity, can make one more susceptible to PIE.
Effective Treatments for Post Inflammatory Erythema
Treating PIE requires patience, as these marks can take months to fade on their own. However, targeted treatments can significantly accelerate the process. A combination of professional procedures and diligent at-home care yields the best results.
Professional Dermatological Treatments
For stubborn or widespread PIE, consulting a dermatologist is highly recommended. They can offer several effective in-office procedures:
- Pulsed Dye Laser (PDL): Often considered the gold standard for treating PIE. This laser targets the hemoglobin in the dilated blood vessels, heating and destroying them without damaging the surrounding skin.
- Intense Pulsed Light (IPL): A broad-spectrum light treatment that can reduce redness and improve overall skin tone.
- Vascular Lasers (e.g., KTP, Nd:YAG): Similar to PDL, these lasers target blood vessels to reduce redness.
- Microneedling: This procedure creates controlled micro-injuries to stimulate collagen production and skin remodeling, which can help repair the damaged vascular network. For a deeper look at treatments that support skin and cellular health, you might find our review on advanced mitochondrial formula insightful.
Topical At-Home Treatments
Consistent use of the right topical products can support healing and prevent new PIE from forming.
- Niacinamide (Vitamin B3): A superstar ingredient for strengthening the skin barrier, reducing inflammation, and minimizing redness. Studies show it can help improve skin’s elasticity and repair function.
- Azelaic Acid: Excellent for reducing inflammation and redness. It’s particularly beneficial for those with acne-prone or rosacea-affected skin.
- Centella Asiatica (Cica): Known for its incredible wound-healing and anti-inflammatory properties, it helps soothe skin and promote repair.
- Vitamin C: A potent antioxidant that can help strengthen capillary walls and support overall skin health.
- Sunscreen: This is non-negotiable. UV exposure worsens inflammation and can prolong the life of PIE. Daily use of a broad-spectrum SPF 30+ is critical.
How to Prevent Post Inflammatory Erythema
Prevention is always more effective than treatment. A proactive skincare and lifestyle routine can minimize your risk.
- Treat Acne Early and Gently: Use proven acne-fighting ingredients like salicylic acid or benzoyl peroxide to prevent lesions from becoming severely inflamed.
- Resist the Urge to Pick: This cannot be overstated. Picking spreads bacteria and causes deeper trauma. If you struggle with this habit, cover active pimples with a hydrocolloid patch.
- Adopt a Soothing Skincare Routine: Focus on barrier-supporting ingredients like ceramides, fatty acids, and the anti-inflammatory botanicals mentioned above. Harsh, stripping products can worsen inflammation.
- Prioritize Sun Protection: As noted, sunscreen is your best defense against prolonged redness and overall skin damage.
- Consider Dietary Factors: While more research is needed, some evidence suggests an anti-inflammatory diet rich in antioxidants may support skin health. For example, comparing the benefits of blueberries vs raspberries can help you choose powerful, skin-friendly foods.
When to See a Dermatologist
If your PIE is severe, widespread, or not responding to diligent at-home care after several months, schedule an appointment with a board-certified dermatologist. They can provide an accurate diagnosis—confirming it is PIE and not another condition—and create a personalized treatment plan, which may include prescription topicals or in-office procedures for the fastest results.
In conclusion, post inflammatory erythema is a common and treatable condition. By understanding its vascular nature, you can choose the right treatments, avoid ineffective ones meant for hyperpigmentation, and take steps to prevent future marks.
With a combination of professional guidance, targeted actives, and immense patience, you can achieve a clearer, more even-toned complexion. For more information on related inflammatory skin conditions, you can read about the symptoms of strep throat, which, while different, also involve a significant inflammatory response in the body.

