Dead Tooth: Symptoms, Causes, Treatment
Dead Tooth: Recognizing the Signs and Saving Your Smile
A healthy tooth is a living structure, powered by a vital nerve and blood supply housed in its pulp chamber. However, when this inner core is severely damaged or infected, the blood flow can be cut off, leading to what is clinically known as a non-vital tooth, or more commonly, a dead tooth.
Understanding this condition is crucial because, left untreated, it can lead to serious complications, including abscesses and bone loss. This guide will walk you through everything you need to know about dead teeth, from the first subtle signs to the most effective treatment pathways.
What Exactly is a Dead Tooth? 🦷
At the center of every tooth is a soft tissue called the pulp. This pulp contains nerves, blood vessels, and connective tissue—essentially, it’s the tooth’s lifeline. A dead tooth, therefore, is one where this pulp has necrosed (died). This necrosis stops all blood flow, meaning the tooth is no longer receiving nutrients or sensory signals.
The process can happen suddenly due to impact or gradually from unchecked decay. Consequently, while the outer enamel and dentin layers may remain intact for a time, the inner tooth is no longer alive.
It’s important to note that a dead tooth won’t simply fall out on its own; instead, it becomes a potential site for infection that can spread to surrounding tissues.
Key Symptoms and Signs to Watch For
Recognizing a dead tooth early can significantly improve your treatment outcomes. The symptoms can vary, sometimes presenting dramatically and other times quite subtly.
Primary Symptoms
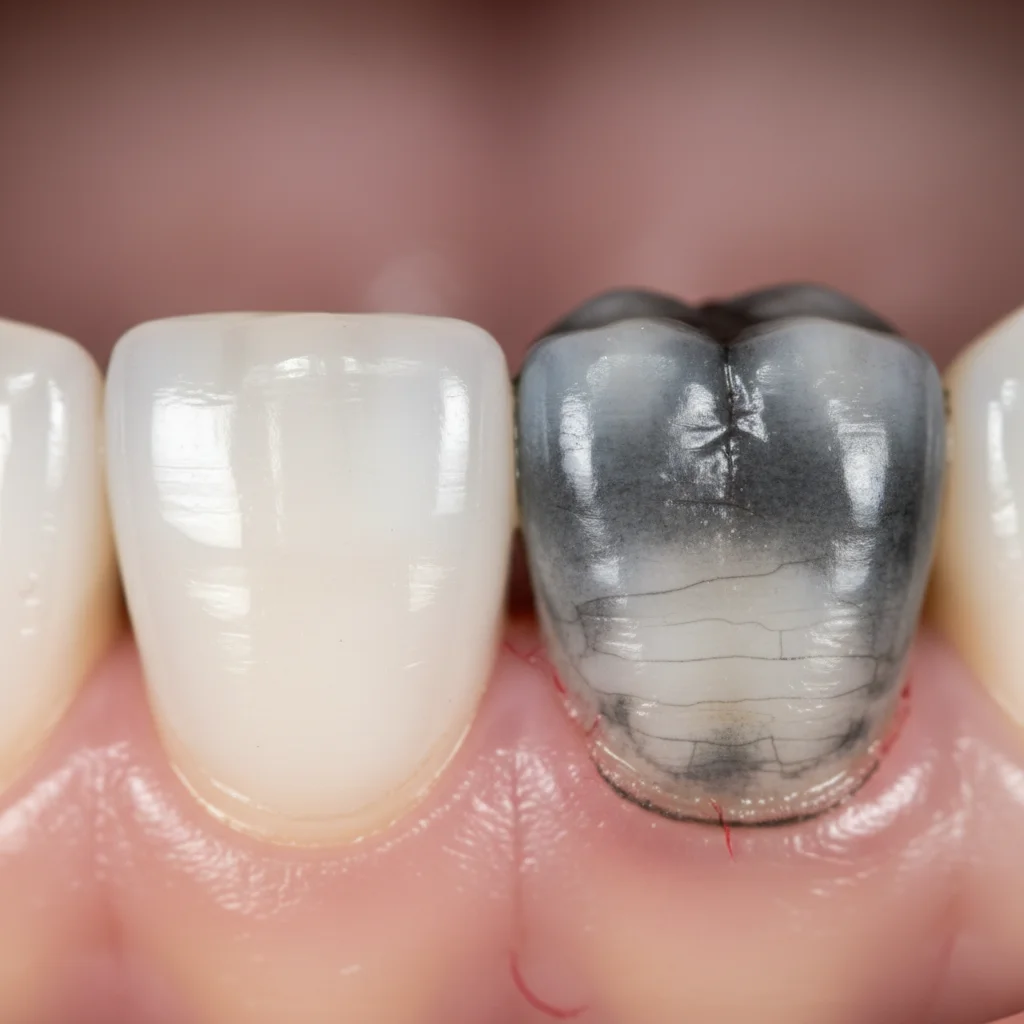
- Tooth Discoloration: This is one of the most common signs. The tooth may turn gray, black, yellow, or brown. This happens because the red blood cells inside the pulp are breaking down, similar to a bruise. The discoloration is often progressive.
- Persistent Pain: You may experience a constant, dull ache or sharp pain, especially when biting down. The pain can sometimes radiate to your jaw, ear, or other teeth.
- Swelling and Tenderness: The gums around the affected tooth may become swollen, tender, or develop a pimple-like bump (called a fistula) that can drain pus.
- Bad Taste or Odor: An infection from the dead pulp can lead to a foul taste in your mouth or persistent bad breath that doesn’t resolve with brushing.
Secondary Indicators
Initially, as the nerve dies, you might feel a significant toothache. Paradoxically, once the nerve is completely dead, the sharp pain may disappear, creating a false sense of relief.
However, the absence of pain does not mean the problem is solved. The infection can continue to spread silently to the jawbone.
What Causes a Tooth to Die?
Two primary pathways lead to a non-vital tooth:
- Physical Trauma or Injury: A significant blow to the mouth from a sports injury, fall, or accident can sever the blood vessels at the tooth’s tip, cutting off the blood supply. The nerve may die immediately or over the following weeks or months.
- Deep Tooth Decay: This is the most common cause. When a cavity is left untreated, bacteria eat through the enamel and dentin, eventually reaching the pulp. This bacterial invasion causes infection, inflammation (pulpitis), and ultimately, the death of the pulp tissue. For more on managing bodily responses to imbalance, you can read about blood sugar levels.
Potential Complications of an Untreated Dead Tooth
Ignoring a dead tooth is a serious health risk. The bacterial infection from the dead pulp doesn’t stay contained. It can lead to:
* Dental Abscess: A pocket of pus that forms at the tooth’s root, causing severe pain, swelling, and fever.
* Cyst Formation: A fluid-filled cavity can develop in the jawbone, damaging surrounding teeth and bone structure.
* Systemic Infection: In rare cases, the infection can enter the bloodstream, leading to a condition called sepsis, which is a medical emergency.
* Bone Loss: The infection can destroy the jawbone that supports the tooth, leading to tooth loss.
Diagnosis and Professional Treatment Options
If you suspect a dead tooth, you must see a dentist promptly. They will typically perform a visual examination, check for discoloration and swelling, and use two key tests:
* Thermal Testing: Applying hot or cold stimuli to see if the tooth responds.
* Percussion Testing: Tapping the tooth to check for pain.
* X-rays: These are essential to confirm the diagnosis, reveal the extent of decay, and show any infection or bone loss at the root tip.
Standard Treatment Pathways
| Treatment | Description | Best For |
|---|---|---|
| Root Canal Therapy | The dentist removes the dead pulp, cleans, disinfects, and seals the inner canals. The tooth is then restored with a crown. | The primary treatment to save the natural tooth structure. It has a very high success rate. |
| Tooth Extraction | The entire tooth is removed from its socket. | Teeth that are too damaged or decayed to be saved, or if the infection is severe. |
| Dental Implant or Bridge | After extraction, these options replace the missing tooth to restore function and aesthetics. | Following an extraction, to prevent shifting of adjacent teeth and maintain chewing ability. |
Root canal therapy is overwhelmingly the preferred treatment because it preserves your natural tooth.
The procedure has a reputation for being painful, but with modern anesthesia, it is typically no more uncomfortable than getting a standard filling. Moreover, addressing oral health is part of a holistic wellness approach, much like considering specific antioxidants for prostate health can be for overall bodily systems.
Can You Prevent a Dead Tooth?
While not all trauma can be avoided, you can drastically reduce your risk from the leading cause—decay.
* Maintain Impeccable Oral Hygiene: Brush twice daily with fluoride toothpaste and floss every day.
* Attend Regular Dental Check-ups: See your dentist for cleanings and exams at least twice a year. They can catch small cavities before they reach the pulp.
* Wear a Mouthguard: If you play contact sports, a custom-fitted mouthguard is essential to protect your teeth from impact.
* Address Dental Issues Promptly: Never ignore a toothache or visible cavity. Early treatment is always simpler, less expensive, and less invasive.
Final Thoughts
A dead tooth is a serious dental condition that requires immediate professional attention. The key takeaway is that the loss of pain is not a sign of healing but often a sign that the nerve has died.
Therefore, if you notice any discoloration, have experienced recent trauma, or have a persistent toothache that suddenly stops, schedule a dental visit immediately. With timely intervention, usually through a root canal, your tooth can be saved, and your smile can remain healthy and intact for years to come.

