Endosteal Implants: In-Bone Full Depth Guide
Endosteal Implants: The Complete Guide to In-Bone Dental Restoration
If you are considering dental implants to replace missing teeth, you have likely encountered the term “endosteal implant.” This specific type is the most commonly used and widely trusted form of dental implant worldwide. Consequently, understanding what they are, how they work, and who they are for is the first step in making an informed decision about your oral health.
What is an Endosteal Implant?
An endosteal implant is a surgical component that interfaces directly with the bone of the jaw or skull to support a dental prosthesis, such as a crown, bridge, or denture. The term “endosteal” literally means “within the bone,” which perfectly describes its placement. These implants are typically shaped like small screws, cylinders, or blades and are made from biocompatible materials, most commonly titanium or a titanium alloy. Because titanium fuses with bone in a process called osseointegration, it provides an exceptionally stable and permanent foundation for artificial teeth.
How Do Endosteal Implants Compare to Other Types?
To fully appreciate the role of endosteal implants, it’s helpful to compare them to the other primary category: subperiosteal implants.
| Feature | Endosteal Implant | Subperiosteal Implant |
|---|---|---|
| Placement | Surgically placed into the jawbone. | Placed on top of the jawbone, under the gums. |
| Common Use Case | Patients with adequate jawbone height and density. | Patients with significant bone loss who cannot have a bone graft. |
| Procedure Complexity | Typically requires a two-stage surgery with a healing period. | Often a single-stage procedure. |
| Stability & Longevity | Highly stable due to osseointegration; considered the gold standard for long-term success. | Relies on gum tissue for initial support; generally considered less stable long-term. |
| Appearance | Not visible; serves as a root for the crown. | A metal framework may be visible under the gums. |
Moreover, endosteal implants are distinct from other tooth replacement options like bridges or traditional dentures because they preserve bone health and do not require altering adjacent healthy teeth.
The Endosteal Implant Procedure: A Step-by-Step Overview
The process for receiving an endosteal implant is meticulous and occurs over several months to ensure optimal integration and healing.
1. Consultation and Planning: Firstly, a comprehensive dental exam, including X-rays or 3D scans, assesses your jawbone density, gum health, and overall suitability. This phase is critical for planning the precise implant placement.
2. Bone Grafting (If Required): If your jawbone isn’t thick or dense enough to support an implant, a bone graft may be necessary. This procedure must heal for several months before the implant can be placed.
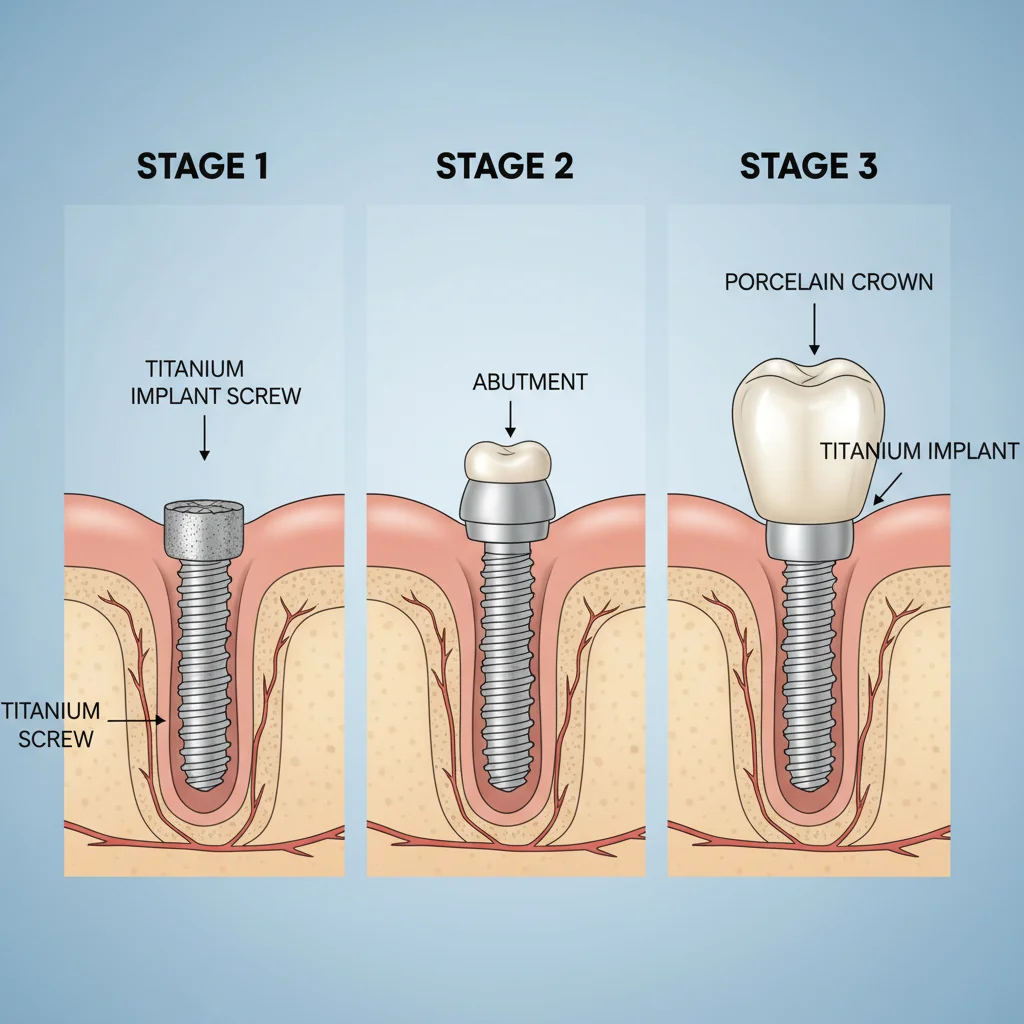
3. Implant Placement Surgery: Under local anesthesia, the oral surgeon makes an incision in the gum to expose the bone. They then drill a small pilot hole and carefully insert the titanium implant post into the jawbone. The gum is stitched closed over the implant.
4. Osseointegration and Healing: This is the most crucial phase. Over the next 3 to 6 months, the bone grows around and fuses with the implant surface, creating a solid anchor. During this time, you may have a temporary denture.
5. Abutment Placement: Once healed, a minor second procedure attaches an abutment—a small connector post—to the implant. This abutment will eventually hold your new tooth. Sometimes this is done during the initial surgery.
6. Crown Attachment: Finally, after your gums heal around the abutment, your dentist takes impressions of your mouth to craft your permanent artificial tooth (crown). The custom crown is then securely attached to the abutment.
Key Benefits and Potential Risks
Advantages of Endosteal Implants
- High Success Rate: They boast a success rate of over 95% when placed by an experienced professional, largely due to the strength of osseointegration.
- Natural Function and Feel: They function like natural tooth roots, providing stability for chewing and preventing bone loss in the jaw.
- Durability: With proper care, they can last a lifetime, making them a cost-effective long-term solution.
- Aesthetic Excellence: The crowns are custom-made to match the color, shape, and size of your natural teeth.
Potential Risks and Considerations
- Surgical Risks: As with any surgery, there is a risk of infection, nerve damage, or sinus problems (for upper jaw implants).
- Requires Adequate Bone: Insufficient bone volume necessitates a prior bone graft, extending the treatment timeline.
- Time-Intensive Process: The full procedure, from placement to final crown, often takes six months to a year.
- Cost: They are a significant investment, though many find the long-term benefits outweigh the initial expense. It’s important to research all options, much like you would when evaluating a wealth signal review for financial tools.
Are You a Candidate for Endosteal Implants?
Ideal candidates generally:
* Have one or more missing teeth.
* Possess adequate jawbone density or are willing to undergo a bone graft.
* Have healthy oral tissues free from periodontal disease.
* Do not have health conditions that severely impair bone healing (uncontrolled diabetes, etc.).
* Are committed to maintaining excellent oral hygiene and regular dental visits.
If you have experienced significant bone loss, your dentist will discuss alternatives like subperiosteal implants or advanced bone grafting techniques.
Caring for Your Endosteal Implant
Long-term success depends on meticulous care. Treat your implant like a natural tooth: brush twice daily, floss regularly (using implant-specific floss if needed), and use an antibacterial mouthwash. Additionally, avoid chewing extremely hard items (like ice or hard candy) and schedule professional cleanings and check-ups every six months. Good overall health supports implant success; for instance, managing blood sugar levels is crucial as high glucose can hinder healing and increase infection risk.
Conclusion
Endosteal implants represent the pinnacle of modern restorative dentistry, offering a permanent, stable, and natural-looking solution for tooth loss. While the process requires a commitment of time and resources, the payoff in terms of oral function, health, and confidence is immense. If you are considering this treatment, the essential next step is to consult with a qualified dental implantologist who can create a personalized plan for your smile.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice. Always consult with a licensed dentist or oral surgeon for diagnosis and treatment. You can learn more about the foundational science of implants through resources like the National Institutes of Health (NIH).

