Gingivitis vs Periodontitis Differences
Gingivitis vs Periodontitis: Understanding Gum Disease Stages
Navigating the world of dental health can be confusing, particularly when terms like gingivitis and periodontitis are used. Many people use them interchangeably, but they represent distinct stages of gum disease with vastly different implications for your oral and overall health.
Understanding the difference is crucial because gingivitis is reversible, whereas periodontitis can lead to permanent damage. This guide will break down the key characteristics, symptoms, and treatments for each condition, empowering you to take proactive steps for a healthier smile.
What is Gum Disease?
Gum disease, clinically known as periodontal disease, is an inflammatory condition affecting the tissues surrounding and supporting your teeth. It begins with bacterial plaque buildup along the gumline. If this plaque isn’t removed through proper brushing and flossing, it hardens into tartar, which can only be removed by a dental professional.
This process triggers your body’s immune response, leading to inflammation and, if left unchecked, progressive damage. Consequently, recognizing the early signs is your first line of defense.
Gingivitis: The Early, Reversible Stage
Gingivitis is the initial and mildest form of gum disease. At this stage, the inflammation is confined to the gingiva—your gums. The good news is that the damage is not permanent because the bone and connective tissue holding your teeth in place are not yet affected.
Key Characteristics of Gingivitis:
* Reversibility: The condition is fully reversible with proper oral care.
* Location of Inflammation: Limited to the gum tissue.
* Bone Involvement: No bone loss is present.
* Primary Cause: Buildup of dental plaque.
Common Symptoms of Gingivitis
You might notice several signs indicating gingivitis:
* Red, Swollen Gums: Healthy gums are pink and firm. Inflamed gums often appear dark red and puffy.
* Bleeding Gums: This is a hallmark sign, especially when brushing or flossing. It’s not normal for gums to bleed regularly.
* Bad Breath (Halitosis): Persistent bad breath can be caused by bacteria in plaque.
* Tenderness: Gums may feel tender or sensitive to touch.
Fortunately, because gingivitis doesn’t involve bone loss, it can typically be resolved with a consistent and thorough oral hygiene routine and a professional dental cleaning. This is similar to how addressing foundational health issues, like supporting your prostate health with proper nutrition, can prevent more serious complications down the line.
Periodontitis: The Advanced, Damaging Stage
When gingivitis is left untreated, it can advance to periodontitis. In this severe stage, the inner layer of the gum and bone pull away from the teeth, forming pockets. These pockets collect debris and become infected. The body’s immune system fights the bacteria, but the enzymes and toxins produced in this battle start to break down the bone and connective tissue that hold teeth in place.
Key Characteristics of Periodontitis:
* Irreversibility: The bone and tissue loss is permanent, though manageable.
* Location of Damage: Inflammation and infection spread to the supporting bone.
* Bone Involvement: Progressive bone loss occurs.
* Primary Consequence: If untreated, it leads to tooth mobility and loss.
Symptoms and Signs of Periodontitis
Periodontitis includes all the symptoms of gingivitis, plus more severe indicators:
* Receding Gums: Teeth may look longer as gums pull away.
* Formation of Pockets: Deep spaces develop between teeth and gums.
* Loose or Shifting Teeth: Loss of supporting bone can cause teeth to move.
* Pus Between Teeth and Gums: Indicates a serious infection.
* Changes in Bite: How your teeth fit together may feel different.
* Persistent Bad Taste: Often accompanies the infection.
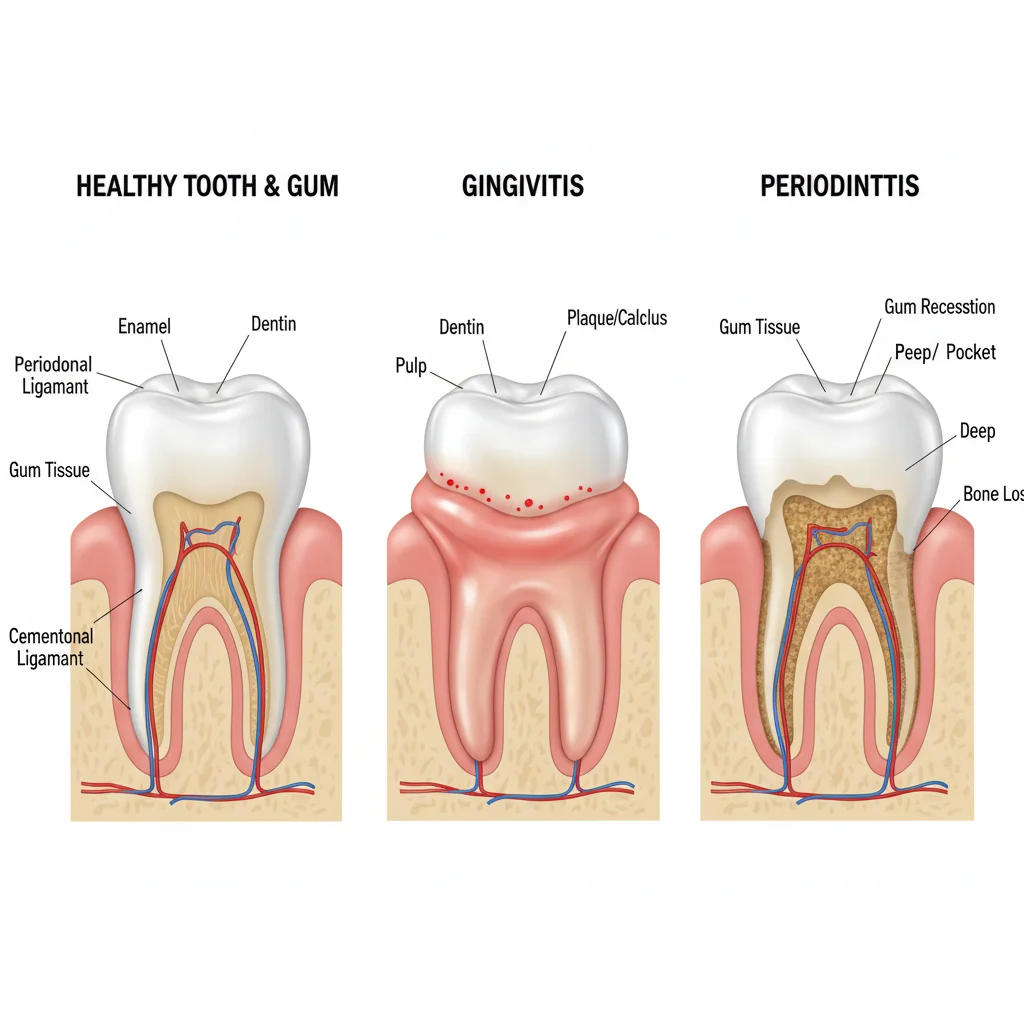
Gingivitis vs Periodontitis: A Side-by-Side Comparison
To clearly visualize the progression, here is a breakdown of the critical differences:
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Stage of Disease | Early, Initial | Advanced, Severe |
| Reversibility | Reversible with proper care | Irreversible; damage is permanent but manageable |
| Tissue Affected | Gum tissue (gingiva) only | Gums, periodontal ligament, and alveolar bone |
| Bone Loss | No bone loss present | Yes, progressive bone destruction occurs |
| Common Symptoms | Red, swollen, bleeding gums | All gingivitis symptoms, plus gum recession, deep pockets, loose teeth, pus |
| Primary Cause | Plaque buildup along gumline | Untreated gingivitis leading to plaque spreading below gumline |
| Treatment Focus | Professional cleaning & improved home care | Deep cleaning (scaling/root planing), possible surgery, ongoing maintenance |
Causes and Risk Factors
Both conditions share common origins but are influenced by various risk factors. The primary cause is always bacterial plaque. However, certain elements can accelerate the progression from gingivitis to periodontitis:
* Poor Oral Hygiene: Inadequate brushing and flossing.
* Smoking/Tobacco Use: A significant risk factor that impairs healing.
* Genetic Predisposition: Some individuals are more susceptible.
* Hormonal Changes: Such as during pregnancy or menopause.
* Chronic Illnesses: Diabetes, cancer, HIV.
* Medications: Some reduce saliva flow, which protects gums.
* Nutritional Deficiencies: Particularly vitamin C deficiency, which is linked to gum health. For instance, understanding blood orange nutrition information can highlight sources of vital nutrients.
Treatment and Prevention Strategies
The treatment approach depends entirely on which stage of disease is present.
Treating Gingivitis: The goal is to eliminate plaque. Treatment involves a professional dental cleaning to remove tartar, followed by excellent daily care: brushing twice daily, flossing, and using an antiseptic mouthwash if recommended.
Treating Periodontitis: Management is more complex. The standard non-surgical treatment is scaling and root planing (a deep clean). This procedure removes tartar and bacteria from tooth surfaces and beneath the gums, smoothing the roots to help gums reattach. In advanced cases, surgical interventions like flap surgery or bone grafts may be necessary. Moreover, consistent periodontal maintenance cleanings every 3-4 months are typically required to manage the condition.
Prevention is Paramount: The best strategy is to prevent gingivitis from starting. This involves:
* Brushing your teeth for two minutes, twice daily.
* Flossing at least once a day.
* Using a therapeutic mouthwash.
* Scheduling regular dental check-ups and cleanings (every 6 months).
* Quitting smoking.
* Eating a balanced diet. Avoiding harmful foods is as important for your gums as it is for other systems; for example, knowing the 10 worst foods for prostate health you should avoid underscores the principle that diet impacts inflammation throughout the body.
The Systemic Health Connection
Research shows a strong link between periodontal disease and overall health. The chronic inflammation from periodontitis is associated with an increased risk of:
* Cardiovascular disease
* Diabetes complications
* Respiratory diseases
* Rheumatoid arthritis
Therefore, maintaining healthy gums is not just about preserving your smile; it’s a critical component of your systemic well-being. For more information on the body’s inflammatory response, you can refer to resources like the National Institute of Dental and Craniofacial Research.
Conclusion: Act Early, Save Your Smile
In summary, gingivitis is a warning sign—a reversible inflammation of the gums. Periodontitis is the consequence of ignoring that warning, resulting in irreversible damage to the structures supporting your teeth. The transition from one to the other is not inevitable.
By recognizing the symptoms early, committing to impeccable oral hygiene, and visiting your dentist regularly, you can stop gum disease in its tracks. Your gums are the foundation of your oral health; protecting them is one of the best long-term investments you can make for your overall health.

